Alex C Spyropoulos, from Feinstein Institute for Medical Research (New York, USA), has presented an anticoagulant treatment strategy to reduce non-fatal blood clots and pulmonary embolism in acutely-ill hospitalised patients, according to clinical findings published in The New England Journal of Medicine. This treatment strategy is associated with almost no critical or fatal bleeding and with a very low incidence of major bleeding.
These results, which were simultaneously presented at the 2018 European Society of Cardiology Annual Congress in Munich, Germany, have the potential to reduce venous thrombosis and non-fatal pulmonary embolism in up to 30% of acutely-ill hospitalised patients. With eight million acutely-ill, hospitalised patients in the USA and another 12 million in the European Union, this novel treatment strategy could potentially prevent tens of thousands of symptomatic venous thrombosis events each year.
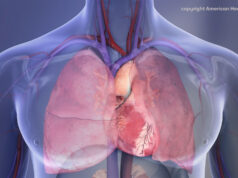
Venous thrombosis is a condition where a blood clot forms due to surgery, cancer, immobilisation and long-term hospitalisation. This clot can travel to the lungs and block blood flow, causing death from a condition called pulmonary embolism. Medically ill patients are at greater risk for developing blood clots while in the hospital and for up to three months afterward. Medications such as anticoagulants are often provided during hospitalisations, but some clinicians and researchers feel these medications could be beneficial for medically ill patients for up to six weeks after hospital discharge when they remain at greatest risk.
Spyropoulos examined whether administering the medication rivaroxaban would help prevent symptomatic venous thrombosis and death related to blood clots after patients are discharged from a hospital. While the trial found the medication was unable to reduce death due to blood clots, the study did identify a potential treatment strategy for those with non-fatal blood clots.
“We were able to reduce instances of non-fatal blood clots and pulmonary embolism by more than half, which shows that the use of direct oral anticoagulants such as Xarelto after the hospitalisation of medically ill patients could help prevent clots from forming,” said Spyropoulos. “Our next course of research is to further identify and refine a post-discharge treatment program which would maximise the net clinical benefit across a defined spectrum of medically ill patients.”
In this double-blind, randomised trial, 6,007 patients were given rivaroxaban and another 6,012 participants provided placebo while in the hospital and for 45 days after discharge. Of those patients only 0.18% in the rivaroxaban group suffered from nonfatal venous thromboembolism versus 0.42% of patients in the placebo group, a statistically significant difference. The incidence of major bleeding was very low and not significantly different between groups (0.28% in the rivaroxaban group vs. 0.15% in the placebo group).
“Dr. Spyropoulos’ discovery of a new treatment avenue for blood clots has the potential to positively benefit patients across the globe,” said Kevin J Tracey, president and CEO of the Feinstein Institute. “He is a respected leader in this field.”