An Australian study currently assessing the Endovenous Valve Transfer Stent (EVTS) may soon be become a larger European trial, if the Australian study is shown to be effective. The EVTS has been developed by Australian company AllVascular for the treatment of deep venous insufficiency and venous ulceration. Over the past few decades the technique of ‘free valve transfer’ has been attempted. While this technique has had some success in the short-term, it is technically difficult and often has long-term failures due to the morphological differences between the veins from the arm and leg. The EVTS essentially allows the same operation to be performed (transferring a valve from the arm to the leg), however the use of the stent allows the vein to be very easily harvested (without stretching, shortening, or twisting of the vein), transferred, and deployed into the host vein.
“The patients in this trial will all have chronic venous ulcers which are well known to have a very serious impact on the quality of life for the patients and a massive burden on the health budget and resources,” commented Dr Mark Philips, general manager of AllVascular. “These patients have very few (if any) treatment options left and this study offers them (and their doctors) a new possibility.”
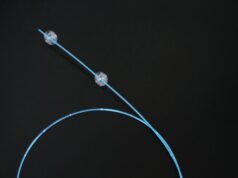
The major feature of the Nitinol self-expanding EVTS is that it contains longitudinal struts that run the length of the stent, with spikes at either end. These act to prevent the stretching, shortening and twisting of the section of vein containing the valve. After the harvesting of the vein (by attaching it to the EVTS), the stent is crimped and placed within a into a deployment sheath. The deployment sheath is inserted into the host vein and the sheath retracted to deploy the EVTS.
According to Philips the company decided to commence human trials following in vivo sheep trials, which were completed in late 2005. “The EVTS was harvested for examination one, three, and six months post-op and was shown to have performed superbly through these trials with no cases of thrombosis, stent migration, infection, or development of valve incompetence,” he commented.
The study is planning to enrol up to 50 patients with chronic deep venous insufficiency and venous ulcers (present for at least six months). The patients will all be examined to demonstrate that suitable venous valves for transfer are present in their axillary veins and that there is a suitable deployment site in the affected leg. All the patients will be followed-up at six weeks, three months and six months. This will involve physical examination and mapping of the size of the venous ulcer (if present), quality of life survey and ultrasound of the valve transfer site to demonstrate that the transferred section of vein and valve is patent and competent. Venography will be used in addition to the ultrasound if the results are inconclusive. The study has thus far enrolled four patients from three Australian centres and depending on the speed of patient recruitment, the results are expected to be published in late 2007.
Separately, according to a study featured in the July 2006 Journal of Vascular Surgery, nonthrombotic iliac vein lesions (NIVLs), which include webs and spurs, have a high prevalence and a broad demographic spectrum in patients with chronic venous disease (CVD). The study was performed by Drs Seshadri Raju and Peter Neglen, from the University of Mississippi Medical Center and River Oaks Hospital in Flowood, MI.
According to Raju, NIVL’s are not rare and are commonly found in the asymptomatic general population and are not often visible in venograms. “The clinical syndrome (also known as May-Thurner syndrome, Cockett syndrome or Iliac Vein Compression syndrome) has been thought to be a relatively rare contributor of CVD, predominantly affecting the left lower extremity of young women,” said Raju. “Our study described the much broader disease profile that has emerged with the use of intravascular ultrasound (IVUS) for diagnosis and analysed stent placement outcome in two specific NIVL subsets that may offer clues to their pathogenic role.” The study indicates that these lesions may be permissive of future development of CVD, and stent placement alone without correction of associated reflux often provides relief in symptomatic patients.
A total of 4,026 patients with CVD symptoms spanning the range of clinical classes were included in the study. IVUS examination was selectively carried out in severely symptomatic patients for specific indications. The results revealed that iliac vein obstructive lesions were found in 938 limbs of 879 patients; 53% of the limbs had NIVL, 40% were post-thrombotic and 7% a combination. Outcome of stent placement totalling 332 limbs in 319 patients in two NIVL subsets, one with and the other without associated distal limb reflux, were compared. Reflux was left untreated in the first subset. The median age was 54 years (range 18-90). Female to male ratio was 4:1 and left to right leg ratio was 3:1.
The study showed that the NIVL lesions in the iliac vein occurred at the iliac artery crossing (proximal lesion) and also at hypogastric artery crossing (distal lesion), a new IVUS finding.
According to the research, venography was only 66% sensitive with 34% of venograms found normal, while IVUS had a diagnostic sensitivity of more than 90%. The following cumulative results were observed at 30 months following stent placement, in the NIVL+reflux and NIVL without reflux subsets respectively: complete relief of pain 82% and 77%; complete relief of swelling 47% and 53%; complete stasis ulcer healing 67% and 76%; and overall clinical relief outcome 75% and 79%. These results are nearly identical between the two subsets even though distal reflux remained uncorrected in the NIVL plus reflux subset.