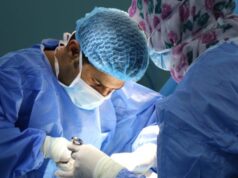
Venous disease-specific quality of life (QoL), as measured by the VEINES (Venous insufficiency epidemiological and economic study)-QoL/Sym, improves significantly after iliac vein stenting for chronic venous obstruction. This is according to the 2021 European Venous Forum (EVF) Prize-winning paper presented by Rachael Morris (St Thomas’ Hospital and King’s College London, London, UK) at the 21st EVF Annual Meeting (24–26 June, online).
“QoL after deep vein thrombosis is severely impaired,” Morris began, noting that studies have demonstrated impairment comparable to that experienced by patients living with other significant cardiovascular, respiratory, and musculoskeletal conditions such as angina, arthritis, and chronic obstructive pulmonary disease.
Post-thrombotic syndrome (PTS) comes with disabling physical symptoms, Morris explained, including leg pain, swelling, venous claudication, and venous ulceration—all factors which, the speaker noted, have a significant impact on patients’ ability to undertake daily activities. “For some patients,” Morris elaborated, “even climbing the stairs is a struggle”.
The presenter stated that PTS has a significant psychological impact as well, and—due to the fact that some patients are left unable to work because of their symptoms—a significant social and economic burden.
The “gold standard” for assessment of QoL and severity of disease in PTS is the Villalta score combined with a venous disease-specific QoL questionnaire, Morris informed EVF viewers. The VEINES-QoL/Sym is one such questionnaire and has been validated “extensively” in several different languages, Morris noted. In addition, it is currently recommended by the European Society for Vascular Surgery.
Morris detailed that the VEINES-QoL/Sym consists of two parts: the VEINES-QoL—a 25-item questionnaire relating to symptoms of chronic venous disease, limitations in activity due to chronic venous disease, the psychological impact of the condition, and the change in leg problem over the last year—and the VEINES-Sym, a subscale of the VEINES-QoL that includes questions relating to symptoms of chronic venous disease only. For both the VEINES-QoL and the VEINES-Sym, a higher score equates to a better clinical outcome, the speaker noted.
The aim of the current study, Morris relayed, was to evaluate change in venous disease-specific QoL after iliac vein stenting for chronic obstruction. A secondary aim was to identify factors associated with improvement in QoL after stenting.
This was a retrospective cohort study, the speaker told virtual attendees. The research team included all VEINES-QoL/Sym questionnaires completed by patients presenting to the St Thomas’ Hospital deep venous outpatient clinic before and after iliac vein stenting between 2016 and 2019.
Morris communicated that the group identified 187 patients who had completed the VEINES-QoL/Sym questionnaire at baseline or follow-up in the study timeframe, adding that they analysed 388 questionnaires in total.
The speaker reported “significant improvement” from baseline for both the VEINES-QoL and the VEINES-Sym. Detailing specific findings, Morris revealed that the VEINES-QoL at baseline was 35.69, which improved to 64.18 at six months postoperatively. The improvement was sustained at 12, 24, and 36 months at 60.52, 60.37, and 55.98, respectively. The VEINES-Sym showed a similar level of improvement, Morris added, increasing to 60 at six months, 52.85 at 12 months, 59 at 24 months, and 50.25 at 36 months. “The change from baseline was highly significant at all follow-up time points,” the speaker remarked.
In addition to improvements in the VEINES-QoL/Sym, Morris informed viewers that the Villalta score also improved. The baseline for this cohort was 14, which the speaker said represents a cohort of patients with “quite severe symptoms” who are “absolutely desperate for something to be done”. At six months postoperatively this was nine, improving to seven point five at 12 months, seven at 24 months, and finally six at 36 months. Again, Morris added, these scores represent a highly significant change from baseline at each time point.
On examination of factors associated with improvement in QoL, Morris reported that the team could identify no factor that was significantly related with an improved QoL outcome, and suggested that larger studies are required to gain some clarity in this area.
Morris concluded that a significant improvement in venous disease-specific QoL, as reported by the VEINES-QoL/Sym, was accompanied by a corresponding clinical improvement in PTS syndrome, severity as measured by the Villalta score, in patients treated at the St Thomas’ Hospital deep venous outpatient clinic between 2016 and 2019.