
Raghu Kolluri gives an overview of elevated central venous pressure—a condition which Kolluri argues is elusive, underdiagnosed and in need of further examination in order to establish its role and relationship to chronic venous insufficiency.
It is not uncommon to encounter patients who are “non-responders” to medical therapies. Venous disease is no exception to this rule. We have all encountered situations wherein even well-planned endovenous therapies do not resolve a patient’s chronic venous insufficiency (CVI) related symptoms. We have learned that obesity and calf pump dysfunction can lead to symptoms consistent with CVI. Our understanding of lipoedema and venolymphatic physiology has also improved over the last decade, leading to increased use of the terms phlebolymphoedema and phlebo-lipo-lymphoedema. However, the prevalence and role of elevated central venous pressure and other related systemic causes that may lead to symptoms similar to CVI are unknown. The reasons for this deficit in knowledge may be manifold. Elevated CVP is an elusive diagnosis, and an underdiagnosed condition. While invasive right heart catheterisation is the gold standard, the more commonly used transthoracic echocardiographic assessment of the right atrial pressure is also quite challenging since most of these patients are obese.
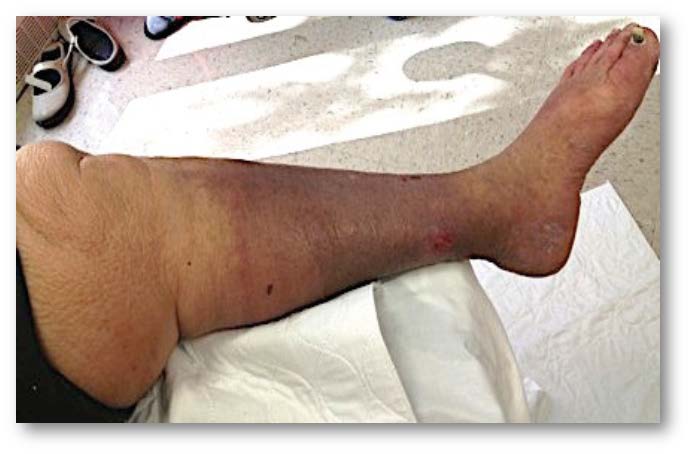
A careful history may reveal underlying risk factors for the development of elevated CVP. These include cardiac risk factors such as ischaemic or non-ischaemic cardiomyopathy, congestive heart failure, diastolic dysfunction, rheumatic fever, intravenous drug abuse, and tricuspid regurgitation, as well as pulmonary diseases including chronic obstructive pulmonary disease, asthma and obstructive sleep apnoea (OSA). Lack of optimal response to compression therapy and proximal displacement of oedema into thighs, buttocks, genital areas and pelvis are clues that oedema is either from lymphoedema or due to a systemic cause or due to elevated CVP. Patients may report shortness of breath with compression garment application or after initiation of the sequential compression therapy. Sequential compression can also result in excessive volume displacement proximally, resulting in hospitalisation from acute right heart failure or pulmonary oedema. Physical examination findings include elevated jugular venous distension, positive hepatojugular reflux, a prominent pulmonic component of the second heart sound and a holo/ pan-systolic murmur of the tricuspid regurgitation in the left third or fourth intercostal spaces. Systolic hepatic pulsations may be palpable in severe tricuspid regurgitation.
To assess the prevalence of elevated central venous pressure in chronic venous insufficient patients, we conducted a prospective descriptive study in our centre. We enrolled 264 consecutive patients referred to the vascular lab with a diagnosis of CVI, between September 2015, and August 2016. All of these patients underwent venous reflux duplex study and a limited echocardiogram to assess elevated CVP. Demographics and other potential risk factors for oedema and CVI-like symptoms were collected. A validated obstructive sleep apnoea risk screening tool called the STOP-BANG score was administered in patients without a history of OSA. We noted a high prevalence of OSA, patients at risk for OSA, and elevated CVP.
Raghu Kolluri is an angiologist in Columbus, USA, and chairman of the VEINS at the annual Vascular InterVentional Advances (VIVA) meeting.












