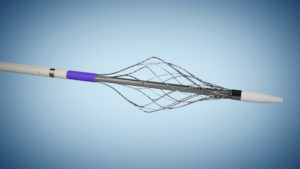
Vetex Medical has announced US Food and Drug Administration (FDA) 510(k) clearance for the ReVene thrombectomy catheter.
ReVene uses dual-action technology designed to de-clot peripheral vessels, such as in deep vein thrombosis (DVT), through wall-to-wall contact in a single session without the use of thrombolytics. The device is expected to be commercially available in the USA later in the year.
“With ReVene, there is the exciting possibility that we may not only make thrombectomy a better procedure for the patient themselves, but also for the healthcare system,” said Stephen A Black (Guy’s and St Thomas’ Hospital NHS Foundation Trust and Kings College Hospital, London, UK). “The device has achieved promising clinical results using minimal passes to remove thrombus, even in difficult-to-treat patients, no need for thrombolytics in most patients, only an overnight hospital stay, and with ease of set-up and insertion. This technology offers the potential to increase procedural efficiency while also improving the cost dynamics of thrombus removal in the clinic.”
ReVene removes clot with a dual-action approach: a dynamic cage separates clot from vessel walls through wall-to-wall contact, while the catheter simultaneously draws clot into the device, where it is macerated and transported out of the body.
According to a Vetex Medical press release, the device is purpose-built for the venous system and safeguards vessel walls and valves by self-adapting to vessel size and physiology. In addition, clot is continuously extracted during the procedure, minimising the number of device passes and creating procedural efficiencies.
Six-month outcomes from the VETEX clinical study of acute iliofemoral DVT patients, the majority of whom had severe disease with chronic clot noted during thrombectomy, showed significant improvements in symptoms, leg swelling and quality of life, with no device-related adverse events or major bleeding reported. The median thrombectomy time was only 23 minutes, and as short as three minutes. In 89% of cases, no thrombolytics were used during the procedure to achieve these results. Data were presented at LINC 2021 (The Leipzig Interventional Course; 25–29 January, virtual) by Gerry O’Sullivan (University Hospitals Galway, Galway, Ireland).












